Study setting and design
This single-arm multi-center feasibility study with a mixed-methods sequential explanatory design was conducted between November 2023 and February 2024 at the Charité – Universitätsmedizin, Berlin and the Immanuel Hospital (IHB), Berlin – Wannsee, Germany. It was carried out and reported in accordance with the CONSORT extension to pilot and feasibility trials34, the Mixed-Methods Article Reporting Standards35 and the IMA31. It received ethical approval from the Ethics Committee of the Charité – Universitätsmedizin Berlin on 14th July, 2023 (EA1/157/23) and was registered in the German Clinical Trials Register prior to commencement of the study (DRKS00032014, 17/10/2023). The study adhered to the principles of the Declaration of Helsinki. The study design and procedure are outlined in detail in the study protocol36.
Eligibility criteria
Inclusion criteria comprised: HCPs, actively practicing medicine or nursing at one of the two study sites, of 18 years or older who completed written informed consent and were proficient in the German language. Exclusion criteria were a current clinical burnout syndrome diagnosis according to ICD-11 (QD85 “Burnout”), pregnancy, or HCPs with solely administrative position.
Recruitment procedure
The research team recruited participants via the hospital´s intranet, project website ( notices, flyers, and informational events at both study sites, as well as by word of mouth. Eligible participants were provided with written study information to review at their convenience. Interested HCPs were contacted by a member of the study team via telephone to confirm eligibility and inquire about their interest in participating. During telephone contact, participants were given the opportunity to ask questions to clarify any uncertainties. Participants were required to provide written informed consent to be enrolled in the study. After enrollment they were asked to fill out the baseline questionnaire and take part in the electrophysiological measures. All participants were clearly informed of their right to leave the study at any moment without giving reasons, and without negative consequences for their employment.
Intervention
Intervention development
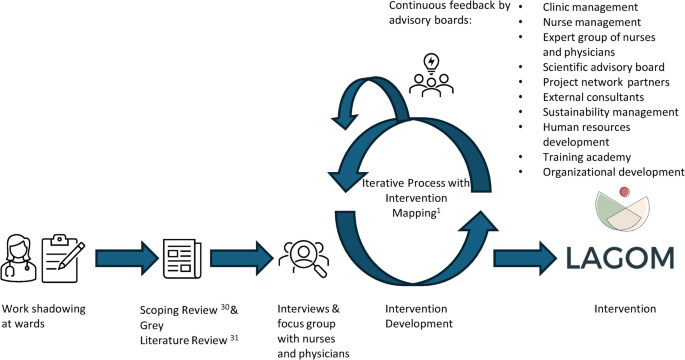
The intervention development followed the IMA by Eldredge et al. (2006)31, a systematic approach based on six steps: (1) Needs assessment; (2) Project outcomes and objectives; (3) Program design; (4) Program production; (5) Program implementation plan; (6) Evaluation plan. The intervention development with preparatory processes is depicted in Fig. 1. The detailed intervention development process will be described in a subsequent publication. The project team consisted of physicians, psychologists, nutritionists, sports scientists, and physical medicine specialists. In addition, advisory boards, such as the chief financial office, clinical and nursing management, and the sustainability management were iteratively involved in intervention development (Fig. 1). A stakeholder group of physicians and nurses gave continuous feedback during the intervention development phase to assure that the needs of HCPs were addressed. Two subject matter experts (one physician and one psychologist with years of experience in mind-body medicine and clinical practice) also gave continuous feedback on intervention content.
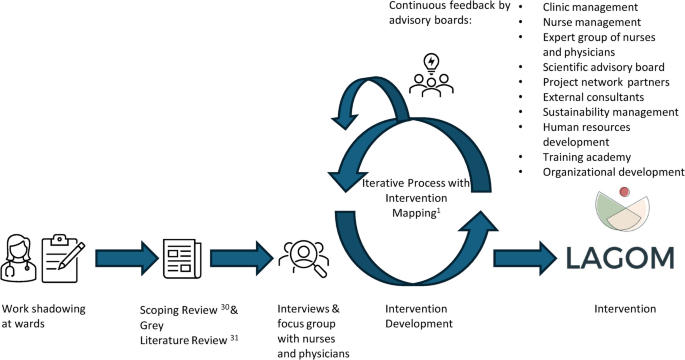
Preparatory work and intervention development process of LAGOM with stakeholders: This figure depicts the development process of the LAGOM intervention, including the stakeholders that were involved in the development process.
LAGOM program
The LAGOM program took place within working hours and its implementation was supported by the clinic management of the two participating hospitals. Works council and employee representative committee of both study sites approved the project. It spanned over a 9-week period with one session per week. The initial and final sessions were scheduled for a duration of two hours each, the subsequent sessions spanned 90 min to accommodate facilitation within regular working hours. Meetings alternated between in-person and online format. Each session adhered to a consistent structure: (1) Commencement involving a movement-based activity for engagement, a moment of silence for centering upon arrival, and brief reflection, (2) Psycho-educational segment covering various topics accompanied by practical exercises and interactive exchange, (3) Relaxation exercise, (4) Conclusion of the session. The weekly LAGOM sessions were led by two physicians who had additional training in mind-body medicine and were experienced coaches, with one physician leading each study site. Teacher training for LAGOM prior to study start and weekly supervision was provided by a member of the core project group (JS), an experienced MBM-trainer. To verify reliability of the course content, trainers received a detailed manual outlining the session structures, together with power point slides for each session to deliver course content to participants. Each participant received a work book, containing all the program content and additional material, such as healthy receipts and additional exercises.
Participants received impulses for organization-directed aspects via e-mail on a weekly basis. HCPs could select relevant activities based on the specific needs and requirements of their wards. Program content is briefly outlined in Table 1.
Data collection
Data was collected before (week 0), during (week 1–9) and after the trial (week 10). Data was assessed using SoSci Survey, a web application for online surveys, as well as through semi-structured interviews. Data was collected and pseudonymized via SoSci to allow for the comparison of baseline questionnaires with post-questionnaires without identifying individuals.
Demographic data
The following sociodemographic variables were assessed: age, gender, height, weight, occupation, full-time yes/no, cultural background (optional), shift work yes/no.
Acceptability and feasibility evaluation
For the feasibility evaluation of LAGOM during working hours, recruitment rate, attrition, completeness of data collection, evaluation of the assessment process, protocol adherence, intervention adherence and safety were assessed. In addition, the intervention was evaluated by the Questionnaire for Professional Training Evaluation (Q4TE), a validated training evaluation questionnaire, as well as a set of five items. An overview of outcomes and definitions is presented in Table 2.
Exploratory effectiveness evaluation
An exploratory effectiveness evaluation was conducted, based on the IMA. The four main components in IMA (quality of life, behavior, environmental conditions and determinants)31 were assessed by the outcomes burnout symptoms, break behavior, implementation of open door appointments, and occupational self-efficacy respectively (Table 2).
Burnout was measured using the Maslach Burnout Inventory, German version (MBI)37the most widely used instrument for assessing burnout in healthcare professionals38. The MBI consists of 22 items grouped into three subscales: Emotional Exhaustion (EE) (9 items), Depersonalization (DP) (5 items), and Personal Accomplishment (PA) (8 items). Each item is rated on a 7-point Likert scale ranging from 0 (“never”) to 6 (“every day”), reflecting the frequency of burnout symptoms. Higher scores on the EE and DP subscales indicate greater burnout, while lower scores on the PA subscale suggest diminished professional efficacy. While the Maslach Burnout Inventory (MBI) is widely used to assess burnout, it is important to note that it is not a diagnostic tool, and there are no universally standardized cut-off scores for defining burnout.
The BSW-5-Rev is a brief and economical scale for measuring occupational self-efficacy, consisting of five items39. It was developed and validated for use with both students and employed individuals. The scale uses a 5-point Likert scale, with higher values indicating greater occupational self-efficacy. In the validation study, the mean score among employed individuals was 3.38, with a standard deviation of 0.44, which can be used as a reference value to interpret the corresponding scores39. For conceptual reasons, the creation of a categorical cut-off does not appear appropriate, according to the authors, as occupational self-efficacy is considered to be a continuous construct39.
Electrophysiological measures
Electrophysiological recordings were conducted at baseline and after the end of the intervention using a Somnomedics SOMNO HD monitoring and recording system. The primary aim was to assess the feasibility of conducting electrophysiological recordings for potential integration into future trials. Due to the complexity of analyses, an evaluation of the electrophysiological parameters will be the subject of a subsequent publication.
Qualitative outcomes
Qualitative data was gathered via open survey questions and semi-structured interviews to follow up on the experiences of participants with the intervention in more depth and help to explain the quantitative data. Questions selected for the interview were based on understanding the complexity of participants´ experience with the intervention and to further explore the answers of participants to the open survey questions (Table 2). Two open survey questions were aimed at capturing the prevailing group opinion (Table 2). A strategic sub-set of three to six participants was targeted for the interviews to capture a wide range of experiences from the two disciplines, hospital units, and study sites. One researcher of the core project team with experience in qualitative research (JB) conducted the interviews. A detailed written record of the interviews was kept by the interviewer.
Data analysis
Quantitative
Sociodemographic data, quantitative survey data and study records were evaluated descriptively using means, standard deviations and percentages as appropriate. Since no confirmatory hypotheses were to be tested within the present feasibility study, all exploratory effectiveness outcomes were evaluated solely descriptively using paired sample t-test reporting mean, standard deviation, Cohen´s d and confidence interval (CI). Statistical significance can be inferred from the CIs, as significance at the 5% level is indicated when the interval does not include the null value. All analyses were performed using the Statistical Package for Social Sciences software (IBM SPSS Statistics for Windows, release 29.0; IBM Corporation, Armonk, NY).
Qualitative
Data was analyzed according to the qualitative content analysis by Kuckartz (2018)41 using the qualitative and mixed methods research software MAXQDA 2022. A deductive approach was used to analyze the data. Two researchers conducted the analysis (JB and MS). The analysis and its results were discussed by the interdisciplinary project team.
Triangulation quantitative and qualitative results
Quantitative results were combined with qualitative findings during the interpretation phase42using qualitative insights and experiences to better understand findings derived from the quantitative data.
Transition to a future pragmatic trial
Based on the results of this feasibility study, the core project team, program trainers and the clinic and nurse management from the two study sites discussed the study outcomes. The fourth author (JS), a qualified counsellor, conducted the discussion. Objectives were to critically discuss the factors and processes linked to participation and satisfaction with the program versus perceived barriers, to provide information for a future pragmatic RCT.
Sample size
Since this was a feasibility study, it did not require adequate power for statistical null hypothesis testing. No formal sample size calculation was conducted beforehand43. N = 30 was set as a target number, based on practical considerations and good practice recommendations for feasibility pilot studies44.
link






