
CNN
—
Kirsten Puccio gave birth to her daughter in August 2020. It was a moment she had both eagerly awaited and dreaded for months.
Upon delivery, Puccio’s doctors were legally mandated to report her to the Massachusetts Department of Children and Families for child abuse and neglect because she was taking methadone, a medication prescribed by her doctor to aid in her recovery from an opioid use disorder.
Puccio had known this would happen. She had gotten prenatal care at a clinic that specialized in treating pregnant people with substance use disorders, and workers there had warned her about the reporting mandate in Massachusetts. Even so, she said, the emotional toll was immense.
“By following doctor’s orders and doing what is recommended medically, you’re then essentially punished,” she said. “No matter how hard you work, how strong your recovery is, how many great positive things you’re doing, you’re still going to be reported for abuse and neglect.”
Puccio says she barely slept for five days after delivery out of fear that officials would take her newborn away.
“I was just in fight or flight mode my whole pregnancy,” she said. “I was panicked the entire time, knowing that upon birth, I was going to have to fight to keep custody of my child.”

Puccio and her doctors had prepared a plan for safe care outlining that safe housing, formula, diapers and other basic needs of the infant would be met at home, so the fight to keep custody of her child was relatively short. The Department of Children and Families closed the case against her in 90 days, but most others are not so lucky, she said.
Drug overdoses are one of the main causes of preventable death among pregnant and postpartum women in the United States. Overdose deaths among this population increased 81% between 2017 and 2020 — resulting in the deaths of more than 1,200 pregnant and postpartum women in 2020.
Yet limited resources and stigma prevent pregnant women who struggle with substance use from seeking or accessing care. Those who do seek care and start taking medications to assist their recovery, like Puccio, are often reported to welfare services for child abuse and neglect under legal mandate.
But in some hospitals, the response is changing.
Mass General Brigham, Massachusetts’ largest health care system, announced last week that it will no longer report suspected abuse or neglect to state welfare officials simply because a baby is born exposed to drugs. Rather, a report will be triggered only if there is reasonable cause to believe that the infant is “suffering or at imminent risk of suffering physical or emotional injury.”
Multidisciplinary care teams who know the family well will meet to determine if there are any concerns about the child not having their basic physical needs (like food, shelter and clothing) or emotional needs (like nurture and stimulation) met. If there are concerns, a report to child welfare services will still be triggered, said Dr. Sarah Wakeman, senior medical director for substance use disorder at Mass General Brigham. However, if those concerns are not present, then exposure to substances on its own will not trigger a report, she said.
“It’s really trying to uncouple this idea of substance exposure as being equivalent to abuse or neglect and instead have our clinicians make an assessment of an individual patient,” Wakeman said.
The system’s approach reflects a growing consensus that punitive approaches to substance use during pregnancy lead to worse medical outcomes for both parent and child and inflict disproportionate harm on families of color and families of low socioeconomic status.
“In most cases, the needs of the parent and the child are actually aligned, and supporting the family unit is the best intervention in terms of child safety and family safety,” Wakeman said.
Change is afoot at many levels. Health systems like the Yale New Haven Children’s Hospital and Boston Medical Center have implemented new drug testing and reporting protocols like those Mass General Brigham announced last week.
States like Connecticut, New Mexico, Washington and Colorado have revised laws to divert substance-exposed infants who are not under threat of abuse or neglect away from the child welfare system. Others, like Massachusetts, have legislation pending that would shield mothers who are taking prescribed medications to treat substance use disorder from child welfare investigations.

At the federal level, the Biden-Harris administration acknowledged that “having substance use disorder in pregnancy is not, by itself, child abuse or neglect” in a report published in 2022.
And a federal bill called the SAFE in Recovery Act, put forth by Sen. Edward J. Markey and others in October, seeks to require consent for toxicology screening of the mother — it’s not a common practice currently — and block states from requiring notification of child welfare officials if the mother is taking a drug in “accordance with the recommendations of the prescribing practitioner” and the health care provider has no other reason to suspect that the child is in imminent danger.
“We can’t accept a reality where parents are being separated from their children, stigmatized or threatened because they are getting the health care they needed, recommended by a doctor and proven to be safe,” Markey said in a news release. “Substance use disorder treatment makes parents and children safer, not less so.”
Laws and interpretations vary
Substance use during pregnancy is linked to negative health outcomes for both the mother and the fetus, according to the US Centers for Disease Control and Prevention. And untreated substance use disorder is a risk factor for child maltreatment; a large percentage of children who come into the welfare system due to reports of abuse and neglect have a parent with a substance use disorder, said Dr. Margaret Lloyd Sieger, associate professor of social work at the University of Connecticut.
However, that does not mean substance use equals maltreatment, she said.
More than 21 million children in the United States live with a parent who misuses substances, according to a 2022 US Department of Health and Human Services report. Not all of those children, Lloyd Sieger said, experience abuse or neglect and need child welfare intervention.
The landscape of child abuse prevention laws and its interpretations varies significantly across states and hospital systems, experts say.
At the federal level, child abuse prevention laws passed in 1974 mandated that child welfare agencies receive notification when an infant was born affected by “illegal drugs”. The Comprehensive Addiction and Recovery Act, known as CARA, removed the word “illegal” from the law in 2016 to mandate notification of authorities anytime a newborn is affected by “drugs”, legal or illegal.
This one-word change is why the law now applies to medication-assisted treatments, such as the methadone Puccio was taking. Theoretically, it could apply to any medication that a pregnant person is taking that affects the infant, including anti-seizure medications and anti-depressants, Wakeman said.
The federal children’s bureau has clarified that a “notification” of drug exposure is not the same as a “report” of child abuse and neglect. However, many states have passed their own laws that equate the two; Massachusetts was among the first to do so in the 1970s, Lloyd Sieger said.
Although these policies desire to protect children, Lloyd Sieger said, research shows that they achieve the opposite effect.
“In states where there are punitive policies, including mandated reporting, birthing people are less likely to access prenatal care, less likely to use medications for opioid use disorder, less likely to use psychotherapy services and less likely to really connect with any health care provider in pregnancy,” she said.
This leads to worse health outcomes for both the baby and the parent, Lloyd Sieger said.
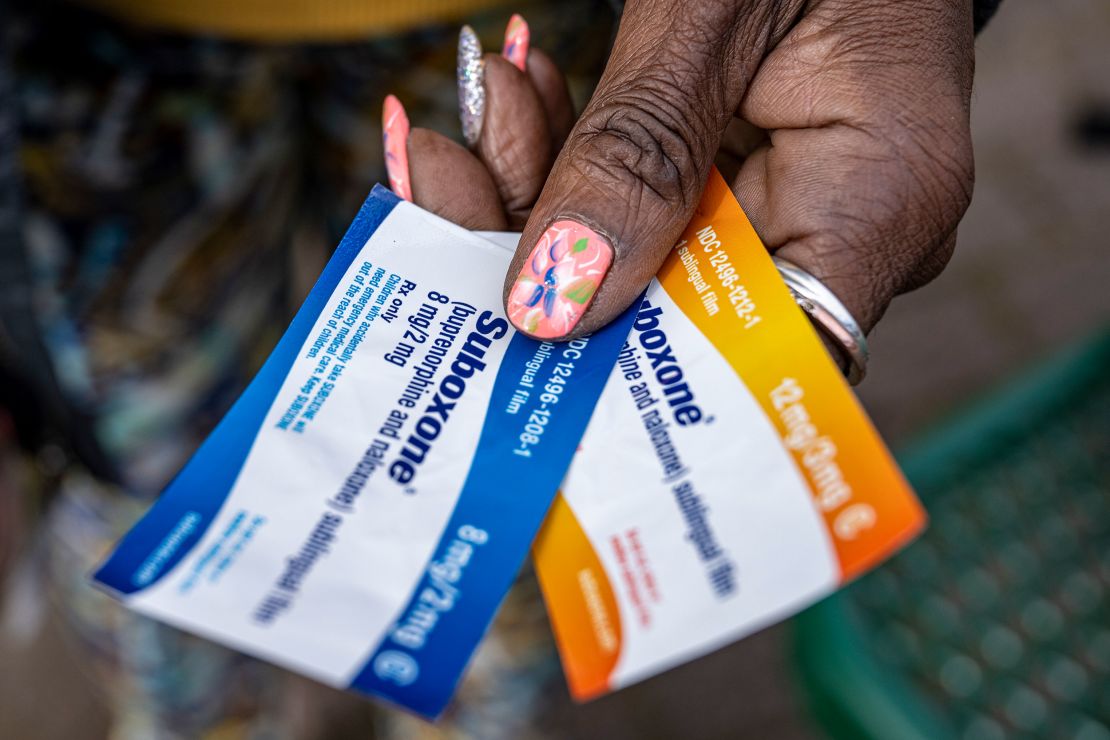
Medication-assisted treatments like methadone and Suboxone (which contains buprenorphine and naloxone) are safe and medically recommended to treat opioid use disorder during pregnancy, according to the American College of Obstetricians and Gynecologists.
In March, the federal Substance Abuse and Mental Health Services Administration issued an advisory about the safety of these treatments during pregnancy and breastfeeding. It also identified that one of the main barriers to seeking care, especially for people of color, is the fear of consequences in states with mandatory reporting.
“When used appropriately, medication for opioid use disorder in pregnancy is associated with a ton of really positive effects on the mom and the baby,” Lloyd Sieger said. “Longer gestation, higher birth weight, better adherence to treatment throughout pregnancy, more frequent prenatal care – just better health and mental health for both.”
Because the medications are opioids, the baby may demonstrate some withdrawal symptoms at birth such as fussiness, body shakes and feeding difficulties, but best practices, like the Eat, Sleep, Console method, have been developed to manage those symptoms effectively, Lloyd Sieger said.
In states where mandatory reporting practices are in place, parents like Puccio who take these medications are automatically reported for child abuse and neglect. Although not all of these reports lead to the removal of the infant from the parent’s care, the involvement of child welfare services is traumatizing in and of itself and can derail confidence in recovery, Lloyd Sieger said.
“The experience of losing custody of a child has been demonstrated in terms of psychological effect to be more traumatic than a child dying,” said Dr. Sharon Ostfeld-Johns, assistant professor of clinical pediatrics and internal medicine at the Yale School of Medicine.
The consequences of punitive policies toward substance use during pregnancy have been especially damaging for families of color and of low socioeconomic status. Inconsistencies in testing and reporting protocols lead to a lot of subjective decision-making that results in significant disparities in outcomes, Ostfeld-Johns said.
Research shows that Black and poor pregnant women are more likely to be screened for drug use during pregnancy and referred to child welfare services than White or wealthier pregnant women, even though women of all races use substances during pregnancy at similar rates. Black children are overrepresented in the child welfare system and Black parents whose infants were placed in foster care are less likely to be reunified with their child, according to a White House report.
Ostfeld-Johns said that observing the differential treatment of mothers based on race within her own hospital motivated her to develop a more objective protocol for toxicology testing of infants. Previously, such tests were ordered inconsistently, leading to biased, often unnecessary referrals to child welfare. The new protocol aimed to eliminate this inconsistency by specifying that the only reason to toxicology test a newborn was if the results would change clinical care – which it very rarely does, Ostfeld-Johns said.
The protocol was implemented in 2021, and it did reduce disparities in testing without causing any increased harm, she said. The objective testing protocol has since been implemented in other hospitals across the nation, including as part of Mass General Brigham’s new policies.
“We want to overall decrease the punitive response to substance use during pregnancy so that people feel comfortable talking to us,” Ostfeld-Johns said. “Then we have a very good understanding of what the use patterns were during pregnancy and how that’s going to affect the newborn.”
Changes have also been made to reporting practices at the state and hospital system levels. Connecticut was the first state to develop a dual-reporting pathway in which anonymized notifications of drug exposure are entered into the system to meet federal reporting requirements, but a separate questionnaire is used to evaluate whether there is concern about abuse and neglect that requires reporting to welfare services.
The notification system was found to divert more than half of substance-exposed infants away from the welfare system, instead connecting families with community services, according to a study by Lloyd Sieger and colleagues that was published in the journal Hospital Pediatrics.
This dual-reporting pathway has become a model for states seeking to distinguish substance exposure from child abuse and neglect.
Colorado adopted similar policies in 2020, requiring providers to report child abuse or neglect only if there was substance exposure and a threat to the child’s well-being, exempting children affected by substances that were prescribed by a doctor.
That policy has been in place for over three years, says Dr. Christine Gold, associate professor of pediatrics at the University of Colorado, but many health care providers are still unaware of the change.
“Unfortunately, we have identified a disconnect between providers ‘on the ground’ and changes happening at a high level without effective communication in a timely fashion,” she said in an email.
Organizations across the state are now working to educate providers about the policy changes and ensure that institutions respond, she said.
Keri McCallum met Kirsten Puccio at the prenatal clinic where they were both patients. McCallum, like Puccio, had struggled with an opioid addiction during pregnancy. She had lost custody of her first child but entered recovery during her second pregnancy.
“Thanks to Suboxone … I changed my life around and got the support I needed,” she said.
Per Massachusetts law, she was reported for child abuse and neglect for taking Suboxone but was able to keep custody of her son and eventually regain custody of her daughter, too.
McCallum and Puccio were both hired as recovery coaches at the prenatal clinic where they met. Reflecting on how isolated they felt during their pregnancies, they decided to found M.I.R.A.C.L.E. Mamas, a nonprofit to help mothers in recovery navigate pregnancy.

“We decided basically to create the space that we wish we had when we were going through dealing with being pregnant and having a substance use disorder,” Puccio said.
McCallum and Puccio said there remains much work to be done to better educate health care providers caring for pregnant patients with substance use disorders. There is also a need to educate expectant mothers with substance use disorders about how the process works and to continue to push for policy and law changes that support pregnant patients in recovery.
“In my dream world, instead of reporting, we should be supporting these families and giving them resources for their recovery journeys,” Puccio said.
link






